June 13, 2018
Early Intervention with Cryopreserved Amniotic Membrane: A Mindset Shift
published on June 13, 2018 by
I’m a firm believer in evidence-based medicine, which is one of the main reasons I’ve always used cryopreserved amniotic membrane (Prokera®) versus dehydrated tissue for the treatment of dry eye disease (DED). The cryopreserved amniotic tissue is processed using the proprietary CryoTek® technology (BioTissue), which has been proven to preserve the biological properties of amniotic membrane and umbilical cord tissue. These biological components that have been shown to play a major role in controlling inflammation and preventing scarring, include the Heavy Chain Hyaluronic Acid/Pentraxin-3 complex (HC-HA/PTX3).
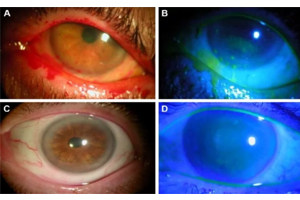
A Mindset Shift: Early Intervention
My approach to treating patients with dry eye disease (DED) is somewhat simple. I typically start by stratifying patients into one of four buckets – DEWS levels one through four. Historically I’ve used Prokera for patients at level three or above, such as those with diffuse punctate keratitis staining or filamentary keratitis. However, in the past year I’ve shifted my approach, and I’m using Prokera more early on and in conjunction with other treatments.
Oftentimes when I see patients in my Dry Eye Center they are further down the road in the progression of their DED due to increased age, comorbidities and other risk factors. To me, the sweet spot for Xiidra® or Restasis® is the mild to moderate patient who is typically between thirty to fifty years old. However, many patients will self-treat or haven’t been given the right therapies, which is why I may see them after their disease has progressed and when they are a bit older.
I still use Xiidra and Restasis as frontline therapies for these patients, but now I also use Prokera in conjunction with these therapies to help accelerate their efficacy, as well as decrease the need for off-label use of therapies like steroids. I have found that this approach helps these medications work faster and as a result my patients feel better quicker – oftentimes within a few days versus months.
Helping Patients Heal Faster
Many physicians reach for Prokera only when things reach that “train wreck” stage with dry eye. As we all know, DED can be labor intensive and rigorous to treat, and we often see patients multiple times and try many different therapeutics. This mindset shift of using Prokera early on and in conjunction with other therapies, helps to make our dry eye clinic more efficient, reduce the number of office visits, and helps our patients heal faster. It’s obviously a profitable niche as well, but Prokera also helps all the therapeutics work better and faster. In my opinion it’s something doctors need to consider using sooner, rather than waiting later when things reach that more advanced “train wreck” stage of DED.
My advice to other doctors who haven’t used Prokera is to just try it. If you’ve tried multiple therapeutics that aren’t working, this is a great alternative and a unique class of treatment. The key is trying it, getting your confidence, and moving forward!
Josh Johnston, OD, FAAO practices at Georgia Eye Partners where he is Clinical Director, Residency Director and oversees the practice’s Dry Eye Clinic, a BioTissue Center of Regenerative Excellence (CORE). His clinical focus is on ocular surface disease, including dry eye and other corneal diseases, and his background includes extensive experience co- managing surgical patients before and after LASIK, cataract and other advanced corneal and refractive surgical procedures.
