DISCLAIMER
The guidance contained herein, is provided for informational purposes only and represents no statement, promise, or guarantee by BioTissue Holdings Inc. or its operating subsidiaries, including BioTissue Ocular Inc. and BioTissue Surgical Inc. (collectively BioTissue) concerning reimbursement, payment, or charges. It is always the provider’s responsibility to determine and submit approrpiate codes, modifiers, and charges that reflect services provided. CPT codes and HCPCS codes are supplied for informational purposes only and represent no statement, promise, or guarantee by BioTissue that these code selections will be appropriate for a given service or that reimbursement will be made to the provider. This information is not intended to increase or maximize reimbursement by a Payor. BioTissue strongly recommends that you consult your individual Payor Organization regarding its relative and current reimbursement policies. For complete indications, contraindications, warnings, precautions, and adverse reactions, please reference full package inserts.
For Healthcare Professionals
Reimbursement Information
Click the links on the right to access the latest resources with coding and reimbursement information for BioTissue’s Innovative Regenerative Healing Human Amniotic Membrane tissue products. For issues with reimbursement, The Pinnacle Health Group is ready to assist.
Neox® and Clarix®
Surgical
To ensure your patient meets their carrier’s medical necessity policy criteria, or to find out if Prior Authorization or Pre-Determination is required, it is recommended that you contact the patient’s payor directly.
Assigned HCPCS code for:
Q4148 | Applicable to Clarix 1K, Neox 1K, Neox RT, per square centimeter
Q4156 | Applicable to Clarix 100, Neox 100, per square centimeter
The Pinnacle Health Group
[email protected]
Phone: 866-369-9290
Fax: 877-499-2986
Hours: Mon. – Fri., 8:30 AM – 6:00 PM ET
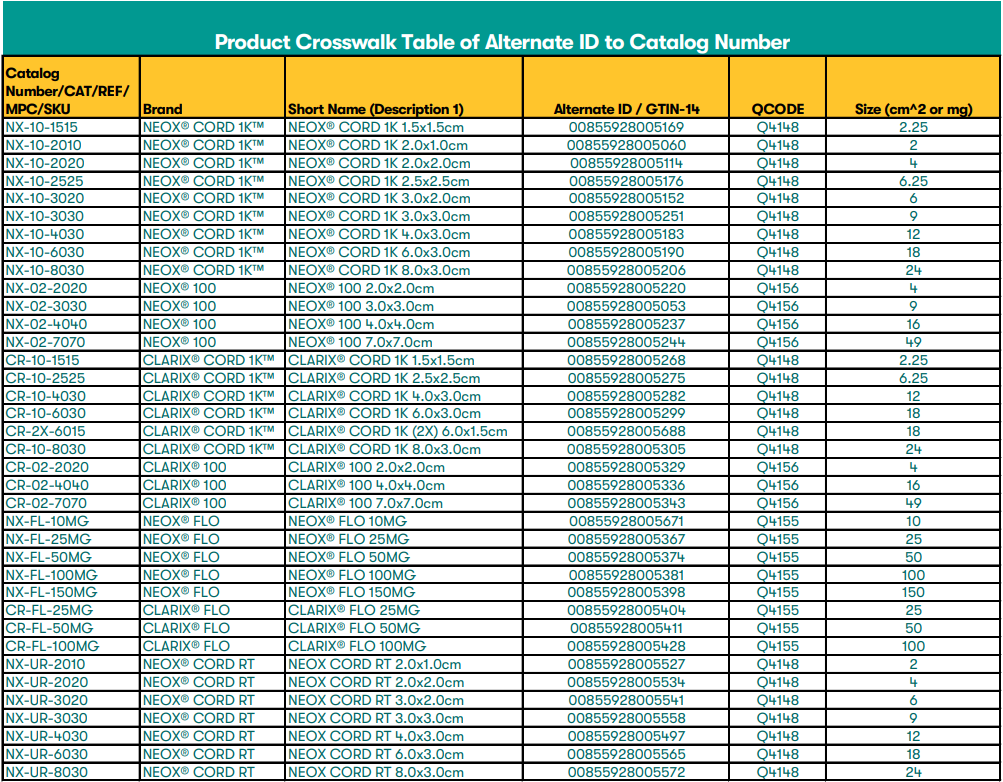
Product Crosswalk Table of Alternate ID (GTIN) and Catalog Number

2026 Surgical Resource Guide - Foot & Ankle
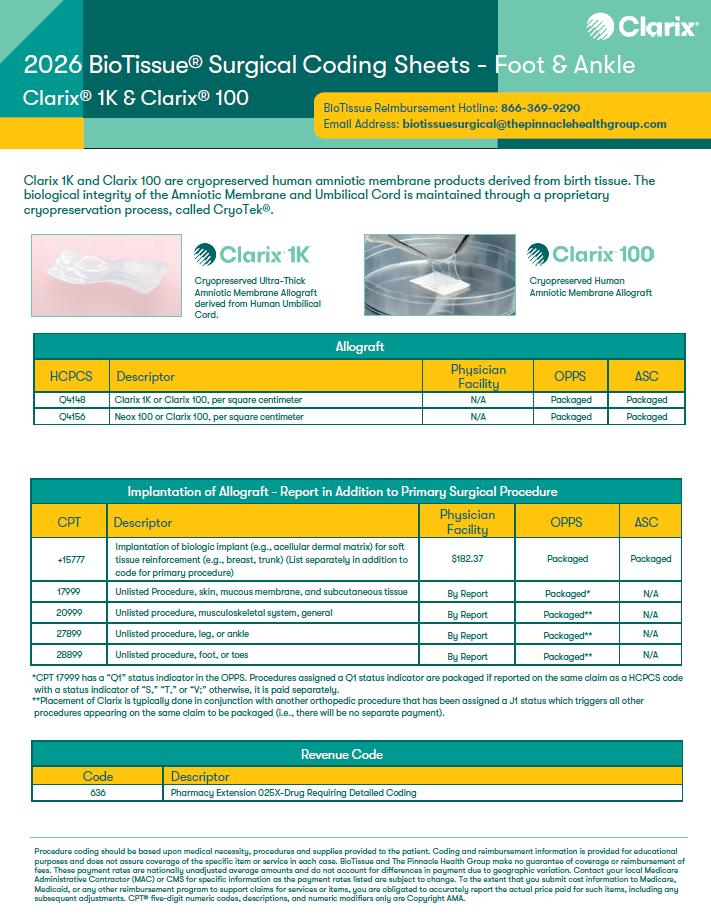

2026 Surgical Coding Sheets - Clarix

2026 Wound Care Resource Guide - Neox
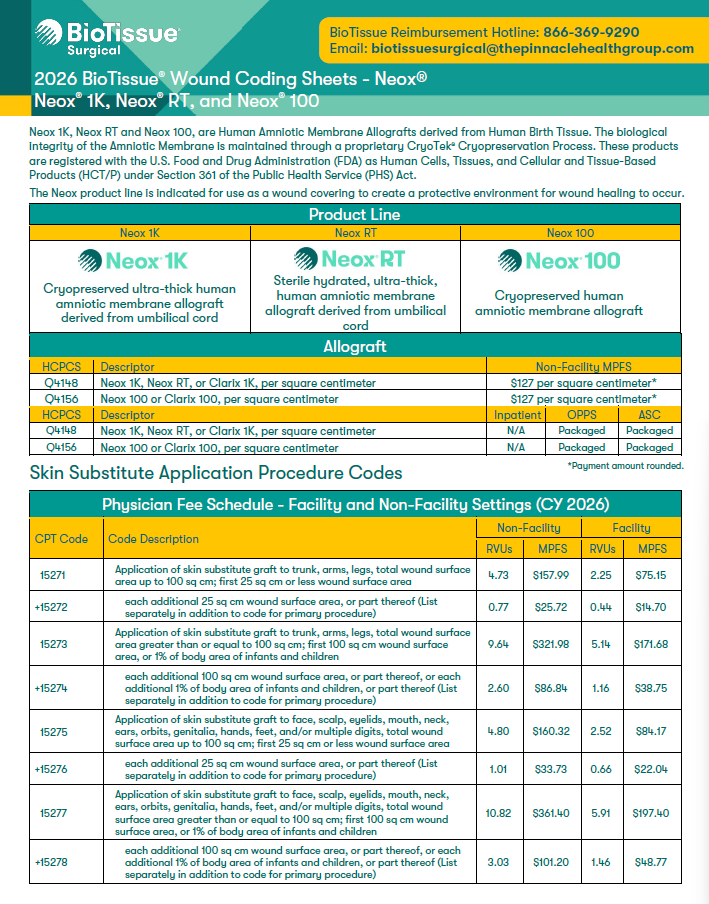
2026 Wound Care Coding Sheets - Neox
Prokera®, AmnioGraft® and AmnioGuard®
Ocular
To ensure a patient meets their carrier’s medical necessity policy criteria, or to find out if a Prior Authorization or Pre-Determination is required, it is recommended that you contact the patient’s payor directly.
Assigned HCPCS code for Prokera, AmnioGraft, and AmnioGuard:
V2790 | Amniotic membrane for surgical reconstruction, per procedure
The Pinnacle Health Group
BioTissue has a Reimbursement Support Hotline which is available by contacting The Pinnacle Health Group.
[email protected]
Phone: 866-369-9290
Fax: 877-499-2986
Hours: Mon. – Fri., 8:30 AM – 6:00 PM ET

2026 BioTissue Ocular Resource Guide
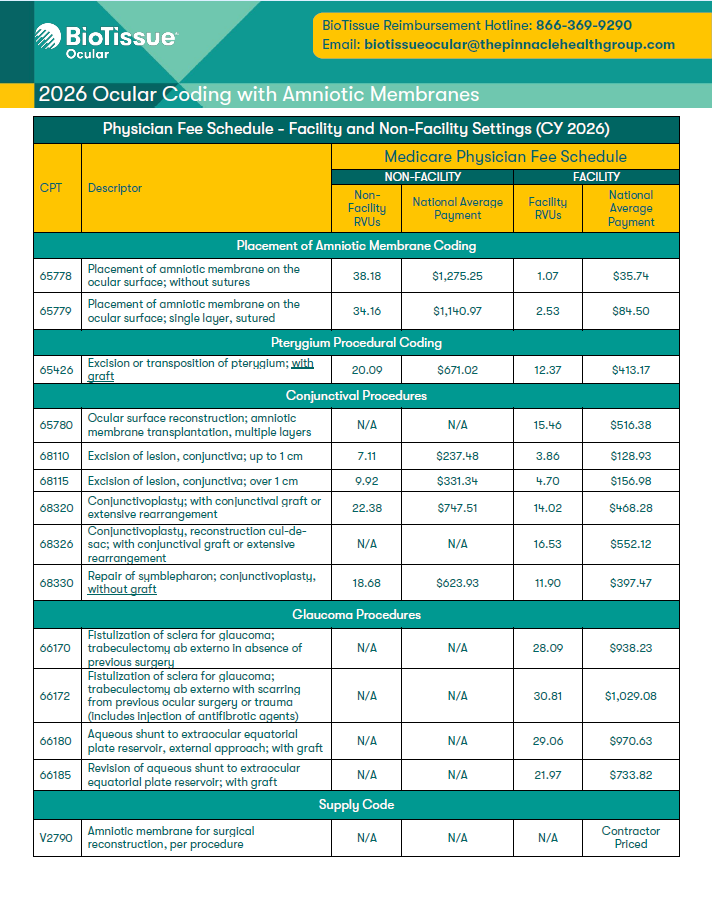
2026 BioTissue Ocular Coding Sheets
For Prokera, CAM360 AG, and AmnioGraft
*Information contained on this page is provided as a reference and for informational purposes only.